Webinar
The State of Our Children’s Health
Time & Location
America’s children are facing an unprecedented storm of challenges to their physical and mental health. The latest research shows that 1 in 25 five years old today won’t make it to their 40th birthday, due in part to unintentional injuries and gun violence. Economic and pandemic-related stresses have had a dire impact on families. Existing health disparities are increasing among Black, Latino, Native American, and other children in vulnerable communities, while LGBTQ youth are experiencing higher rates of bullying, social stigma, and depression.
For this webinar, leading experts in unintentional injury, health equity, and children’s physical and mental health explored the scope of these issues, solutions, and new approaches to protecting our children and improving their health and well-being.
Speakers discussed:
The latest research on the increasing mortality and unintentional injury in children and the policies and social issues driving these trends, along with possible solutions and methods for addressing the problem.
Child poverty, the need for health equity among children, and the impact and value of policies such as the child tax credit
The state of children’s mental health and community-based approaches to supporting improved behavioral health.
1:16
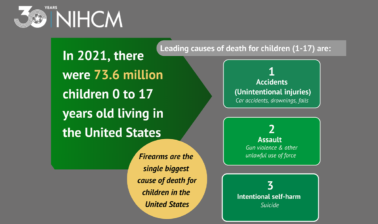
Thank you. Welcome everyone, and thank you so much for joining us this afternoon. I'm Sheree Crute Director of Communications at the National Institute for Health Care Management Foundation, NIHCM. Today we are here to explore what many public health experts consider to be a time of crisis and child health. Across the United States, children are facing multiple unprecedented challenges to their health, safety, and well-being. A widely reported recent study found that 1 in 25 American 5 year olds are not expected to live to age 40. Firearms are now the single largest cause of death for children in the United States, followed by overdoses and dangerous driving. Many young people are also living with trauma linked to the pandemic.
2:05
In addition to the more than 200,000 children who lost their parents or caregivers to COVI- 19, existing economic and social hardships and disparities affecting children have increased as the country attempts to get back to normal.
2:21
The expert speakers we are fortunate enough to have today, with us today are going to share some of the latest data and model approaches to understanding the full impact of these important issues, as well as effective approaches and solutions to protecting and improving the health of our children.
2:41
Our panelists are leaders in the latest research and programming, intended to address unintentional injury and child mortality, the impact of discrimination, and a lack of health equity on children and child mental health.
2:57
Before we hear from them, however, I want to thank ... President and CEO, Nancy ..., and our NIHCM team, who helped to convene today's event. You can also find full biographical information for our speakers along with today's agenda and copies of their slides on our website. We also invite you to join the conversation on social media using the hashtag children's health.
3:21
After our speakers have completed their presentations, we will have a brief Q&A, if time permits.
3:29
And now I would like to introduce our first panelist, Stephen H Wolfe. An MD.
3:35
MPH is a leading researcher on Child Mortality, a senior fellow at American Progress, and a Professor of Family Medicine and Population Health at Virginia Commonwealth University, School of Medicine, where he is the founding director of the Center on Society and Health. And now holds the sea Kenneth and Diane, right? Distinguished Chair in Population, Health and Health Equity, is a leading expert on child injury mortality and the lead author of a recent JAMA viewpoint, the new crisis of increasing all cause mortality in US. Children and Adolescence. Doctor ... Career has focused on raising public awareness about social, economic, and environmental commission conditions that shape health and produce an equities. He will discuss the latest data on child mortality and ways to address the issue in the United States. Welcome, doctor Wolf.
4:30
Sheree, It's my pleasure to be here, and good afternoon, everyone.
4:33
Good morning, if you're joining us further West, I'm just going to take a few minutes to talk with you about.
4:41
An alarming trend that we are seeing in death rates in America is children and teenagers.
4:47
It's not a cheerful topic, but I think it really raises the alarm about the trend that the country is currently experiencing.
4:55
Let me back up just to put this in context a little bit.
4:58
We have a longstanding problem in the United States regarding our life expectancy.
5:03
For some years, as you can see on this graph, the rate at which life expectancy has increased in the United States has been slower than in other industrialized countries, and then after 2010, our life expectancy basically flatlined and we stopped seeing increases altogether.
5:20
And you might think this had something to do with the death rates affecting our children, but it actually did not.
5:28
This trend advice expectancy was being driven by rising death rates in young and middle aged adults, 25 to 64 years.
5:36
This has been an alarming trend, has been concerning public health experts for the past decade.
5:43
But during all that time, the one bit of good news was that death rates on either end of the age extreme for young people and our elderly.
5:52
We're going down and they're going in the right direction.
5:55
That was all true up until the Cove at 19 pandemic. obviously, death rates in the elderly increased significantly during the pandemic because older adults were more vulnerable to the disease.
6:07
We saw that the trend in children would continue, too.
6:12
Continue to decline.
6:14
Unfortunately, the news is not good, and so let me give you some background.
6:18
As I said, the original concern was in middle aged adults. Then, later on, the research evidence began to indicate that young adults are being affected.
6:27
But in the pediatric population and here, you're seeing death rates for children ages 1 to 19.
6:34
You can see that up until about 2014 or so, we were seeing steady progress of lowering mortality rate mortality rates in males, shown here, and females here.
6:46
As the pandemic was approaching the years leading up to the pandemic, we saw a concerning trend where that decline seemed to be flatlining.
6:56
But it was during the recent two years during the covert 19 pandemic when we saw a sudden and unprecedented increase in all cause mortality rates. When I say all cause mortality rates, I mean, deaths from everything.
7:10
And basically, what we saw during the years, 2020 and 21, was a 20% increase in all cause mortality, As I'll show you later, this degree of increase has not occurred for at least a half a century, and possibly since the Spanish flu pandemic.
7:29
What's responsible for that increase? You might think it's coded 19, but it actually was not covered 19, played a marginal role in this increase.
7:37
What actually was driving it was an increase in deaths from injuries, and you can see that on this graph, what the graph is showing you in the blue lines are death rates In young males and nail use, the solid line, our guests from injuries, the dashed blue line are deaths from non injuries which basically refers to medical conditions.
8:00
The red line is for females, The solid red line showing injuries for females, The dashed red line, non injuries for females and so several things, jump out at you of this slide. First off obviously is the high injury rate among males.
8:17
What you can also see, though, is that in general, up until the pandemic, the injury death rates were decreasing.
8:25
But then they, they underwent a significant increase during the years of the pandemic.
8:32
Now, one might think that this was something that had to do with Cobalt 19, as I mentioned, it played a relatively small role. In fact, the absolute increase in injury mortality that we saw during 20 and 21 was 12 times higher than the death rate from Kobe.
8:51
And it was basically the four causes, shown on this slide, that were driving that suicide, homicide, accidental drug overdoses, and motor vehicle crashes.
9:02
Those four causes were mainly responsible for this reversal in all cause mortality, And as I'll talk about in a few minutes, this is a very tragic turn of events because it basically means that these four causes are outweighing all the lives that have been saved by advances in pediatric medicine and injury prevention.
9:21
We saw in, in looking at this data however, that, this was not initiated by the Kobe 19 Pandemic in all.
9:29
But for all, but the last case, suicide, homicide and drug overdoses, the problem began before the covert 19 pandemic, it's just that the pandemic exacerbated.
9:39
So let's take a look at the data.
9:41
Suicide rates, this is in each group, 10 to 19.
9:46
I've broken it down by race, ethnicity, ethnicity, for an important reason that the following speakers will elaborate on, which is that the exposure to these risks is not even across our youth.
9:58
That use of color or very often have disproportionate exposure to these risks, but not always so.
10:04
So, here, what you can see with suicide is, first of all, that this has been on the rise for many years. In fact, suicide rates among our youth in America have been increasing since 2007, so more than 15 years of increasing suicide rates.
10:20
You can also see that is the white population that has experienced the highest suicide rate.
10:26
At least seemingly. so, but there's an important group not shown on this slide, that's Native American youth.
10:32
If we add them to the slide, it looks like this. It basically suppresses all the other curves because the suicide rate is so high among American Indian and Alaska Native youth.
10:44
You will see, though, that the line is rather erratic for this population, and that statistical noise is created by the fact that the number of American Indian use is smaller in terms of population size than other groups in the United States.
10:59
So are mortality rate estimates are a little bit more variable.
11:04
I've added a trend line to give you a sense of it, but it's partly because of this reason that I will not always be showing data for the name of Native American youth.
11:13
But it's important to emphasize that, with all that statistical noise set aside, you can clearly see that their suicide rates are horrifically higher compared to other youth homicide rates. Those have been on the increase since 20 13 in the United States.
11:31
Here you can see that the homicide rate in the among black youth is much higher than it is among white and Hispanic youth.
11:39
And this this is a pretty dramatic difference in in death rates.
11:45
Non hispanic black youth accounted for about 63% of the homicides that occurred at ages 10 to 19.
11:53
The rate that they experienced homicides is six times that for Hispanic and more than 20 times that of a non hispanic White and Asian use.
12:04
If you just aggregate this bisects, knowing that males are more at risk than females, it turns out that Black males, ages 10 to 19, are 61 times more likely to die in a homicide than white females of the same age.
12:22
And we'll talk a little bit about what factors may be responsible for that.
12:26
Firearms We've talked about suicide and homicide, Firearms account for a huge proportion of these deaths.
12:33
In fact, firearms accounted for about half of the increase in all cause mortality that we saw during 20 and 21, 21.
12:41
Taken together, this graph shows all of the deaths related to firearms broken out by race and ethnicity.
12:49
And as you can see, black youth experienced a larger proportion of these deaths.
12:55
But you see also that, again, the American Indian and Alaska Native population experienced a very large number of deaths and increases during the years leading up to the pandemic.
13:08
Now, the other factor that has entered onto the scene is drug overdose deaths, The opioid epidemic exposed white youths to increasing rates of deaths from drug overdoses for many years.
13:20
So you can see on that red line on the graph, the fact that for the decade preceding, the pandemic and more white youth and adolescents in particular, were experiencing, drug overdose death rates had a considerably higher rate than Black and Hispanic youth.
13:37
But as we've seen in the adult population, the opioid epidemic has, has hit people of color very hard in recent years.
13:46
The increased access to fentanyl and other synthetic opioids has caused a market increase in drug overdose deaths rates among people of color in the adult population. And now what we were seeing in the years just before the pandemic is that this trend was reaching down into teenagers where we're starting to see an increase in drug overdose deaths rates among Hispanic and black use.
14:09
And during the pandemic, you can see that basically caught up with the white death rate and basically that rate is now statistically equivalent.
14:20
The fourth category that I mentioned is car accidents. And for the most part, this has been a public health success story.
14:26
Death rates, If you look on the left-hand side of the graph, have been plummeting from car accidents due to successes in preventing auto injury deaths using occupant restraints, like car seats and seat belts.
14:41
Airbags, other design features that have made cars and roads safer have produced a remarkable reduction in death rates.
14:49
During the Cove in 1009 pandemic, we saw a sharp increase in car accidents and fatal crash fatalities.
14:56
Here, you see the death rates among youth ages 10 to 19 and what's remarkable about this?
15:03
Again, much like the story with drug overdoses, is that for many years it was white youth who were most likely to die in car accidents.
15:11
But in recent years we've seen a surge in deaths from car accidents among Black and Hispanic youth, and and and also the Native American youth that has matched that and surpassed that of the white population.
15:26
Again, the same curve, I'm adding in the data for Native American use, and you can see that they are the racial group that has the highest likelihood of dying in car accidents, of all categories of use, by race and ethnicity.
15:44
So we say that the carbon 19 pandemic didn't start, those are three of those four causes, and they began years earlier, but accord fuel on the fire. It really exacerbate these trends.
15:56
As you can see, injury mortality overall rose by 23%, just in the year between 2019 and 2020.
16:05
Homicide rates declined by 39% drug overdoses by 114% car accident deaths by 16%.
16:13
Even in younger children, we saw an increase in injury deaths, uh, and two thirds of that was caused by injuries.
16:22
So I just want to pause for a minute, stop talking with all the jargon to explain in plain English what we mean when we say there's an increase in all cause mortality.
16:32
All cause mortality, meaney death from all causes, is a bit of a tug of war between causes of death, where we see progress in lowering mortality rates, and other causes of death, like the ones we've just been talking about, that are causing an increase in all cause mortality rates.
16:49
In general, the first category has won out among our youth.
16:53
That is the progress that we have made, in lowering death rates, has produced a general trend of decreasing all cause mortality. This is a graph that goes back to 1968.
17:05
And you can see that the trend line has clearly been in the area of progress.
17:10
Pay attention right here to what happened with the trim line, This is the way it's supposed to have kept going in recent years.
17:16
Because this increase that we've been talking about in today's talk, means that something has really risen to such a high rate of deaths, causing so many deaths among youth that it is. It is offsetting all the progress that has been made in other categories. And it's been a remarkable amount of progress.
17:34
Progress in the prevention of the disease through the introduction of antibiotics and vaccinations, progress in treating diseases that were the leading causes of death in children.
17:44
Like childhood leukemia.
17:46
Progress in preventing injuries from car accidents, fires, drowning, and so forth.
17:52
A massive amount of lives gained in the end, in young Americans, because of this progress.
17:59
However, what this recent increase in all cause mortality means, is that all of that progress, at this point, is now being offset, by the massive death toll caused by those four causes.
18:11
And so it really makes us focus on three areas that I think are really huge priorities.
18:17
one that's obviously jumping off the screen as you watch these data, is a mental health crisis in our youth.
18:23
The fact that suicide rates have been increasing since 2007 is indication enough, but we already knew about increasing issues of stress, depression, and other mental health challenges facing our young people which the pandemic only exacerbated.
18:39
It's not only a problem that we have root causes responsible for their mental health issues, but also adequate degree of mental health services for young people to provide help.
18:52
Our mental health system is inadequate in the United States is particularly inadequate for the pediatric population, especially, those living in rural areas.
19:01
The second major policy issue coming off of this data is the role of guns.
19:06
Firearms accounted for the vast majority of this increase in all cause mortality.
19:11
As I mentioned earlier, it is now the leading cause of death in children, Past car accidents, and now is the most likely reason our young people are destined to die.
19:21
Then ultimately, we have to confront the issue of inequity and marginalization.
19:27
The disproportionate increase in homicide rates, and other kinds of injury rates among certain racial and ethnic groups, and in low-income communities across our country.
19:40
Really has to do a lot with history and policies and structural factors that have expose those neighborhoods and those populations, two generations of marginalization and cutoff opportunities for social and economic mobility, and better health.
19:59
And that have resulted in tremendous stresses that manifest themselves, in some cases, through self harm, in terms of suicide and other kinds of self damage And violence that that ultimately can lead easily to conflict.
20:17
If you combine that kind of stress and conflict with easy access to guns and increasingly lethal guns as is the case, now, it's a toxic mixture leading to this dramatic increase in death rates.
20:32
I want to make one final point before I pause for the following speakers to emphasize that we're hearing a lot of the news about mass shootings.
20:42
And then the deaths of young people at schools, due to some of these mass shooting incidents.
20:48
And as and like any parent, I am horrified by the news of these mass shootings and seeing the scenes on our television screens.
20:58
But as an epidemiologist, I must tell you that the death toll from guns that we're talking about is not coming from mass shootings, primarily, it's coming from shootings that are occurring: one at a time, every day in communities across this country.
21:15
You'll hear on your evening news about a shooting or multiple shootings that have occurred during the day in your community.
21:22
Many of those involve our youth. And they're adding up to such a massive number that it's producing this shift in all cause mortality, that I'm telling you about.
21:31
So with that, I'm going to pause and turn it over to my colleagues.
21:37
Thank you for your attention, you so much actual, for a very difficult, very important discussion, and what we must do to address rising child mortality or discussion of inequities.
21:51
This is a perfect transition to our next speaker, ... PHD. Doctor Rocha is a research professor in the Department of Public Policy, a fellow at the Frank Porter Graham Child Development Institute, and the founding director of the Equity Research Action Coalition at the University of North Carolina Chapel Hill. She leads projects and initiatives focused on ensuring that minorities, children, and children from low-income households, especially black children, are thriving.
22:24
Her work is focused on ensuring excellence for young diverse learners, especially black children and their families through the intersection of antivirus, anti racist, culturally grounded research programs, and policy. Doctor Rocha will help us understand the role racism and other systemic inequities play in the well-being of Black and Latino, Native American, and other children from minority communities. Doctor Rocha, welcome, thank you.
22:53
Thank you so much, Sherry. I'm so glad to be here with you and with everybody else. And thank you, Sherry and obviously Mcmath for really providing this gray space.
23:02
Let's start much. children's health and written large, of course, getting I'm Erica, my pronouns. Are she, her, hers.
23:09
I just wanted to say that I'm going to talk a bit about the impact of ... health. And I want to show to take them in advance and protection, promotion, and preservation policies. And I want to just take a moment. Can you go to the next slide, please, for me?
23:27
Thank you, And I'm very tensioned about putting Black on my slides. Especially, I grabbed my work in black children, black families in black communities, but also recognize that many minority communities, including our Latino community, are Asian American Pacific Islanders are native community, even, including our LGBTQ rural, and many other communities are really impacted by racism and other systemic inequities. And so, for me, it is important that, as a center, my work on black children, families, they also recognize and work with other organizations who may focus on other sort of subgroups and other populations.
24:03
So, what I just wanted to briefly do is, next slide, please, Is to just share a little bit about the Equity Research Action coalition. And then also just because they'll give you a sense of, you know, the lens that I'm bringing to the work and the conversation. And we'll have following our remarks. So, just, again, briefly, the equity, which actually coalition. And there's a QR code there. Feel free to use your phone or a computer. You can sort of go to a website. And, really, I just want to highlight that we're trying to really focus on co construct an action, or research and evaluation, work practitioners, policymakers, advocates, et cetera, to really support the optimal development of black children and other children for marginalized communities. Again, like our Latino native, actually, disability children living in poverty. Really starting from prenatal through early childhood, so really through that, created through age eight, H 10 Space.
24:52
And I would argue that we're really working at the intersection of research, practice, and policy.
24:57
We're using what I call, the two frameworks of anti racism. Cultural.
25:02
one is recognize the system of inequities is baked into so many things from health care, labor, markets, education, et cetera, but also recognize that many communities of color, many mortgage communities really have a wealth of assets from their family to day communication. To send me things that we often overlook as. We look at obviously the remnants and the travesties brought on by structural racism brought on by systemic inequities in many other dehumanized and policies and programs that impact, you know, disadvantaged communities. And so really try to make sure that we're bringing those two length and trial work.
25:42
Next slide, please.
25:43
And really, we do that through really, and, again, as I said, we do really around the early years to look at our research and evaluation. Holistic perspective does not just about what it's horrible happening, but what are the other assets that our children are bringing, that early care education providers, or bring it in a way that really honors the owners of humanity to really try to identify, what policies are actually actionable? They're actually happened in that extra at least reduce the disparities that we see in particular between black and white communities or black and brown communities in which means you're trying to really identify, what are those policies that really seem to make a dent in the health?
26:23
Again, when I think about health, I think about, well, issues of mental health, physical health, all the sort of writ large health issues, but also issues around wealth, right, in terms of income, poverty, but also wealth and asset development and also ask the education from birth all the way through graduation.
26:41
So what are the policies that really help to reduce those gaps in access, but also experiences and outcomes? And then we also think about mentoring and training. Because in the end of it, you know, there's only one of me right when a doctor Wolf White shirt, right? So how do we make sure that we continue to mentor and train people to really connect the dots between research, policy, and practice, and really translated, which is the final part of our larger work? Is that to really make changes in society, particularly around issues of racism, inequities? We have to begin to change the water and the conversations, and make sure that people understand, what are the economic ramifications? Well, we don't address racial discrimination. What are the ramifications wouldn't address health inequities? Everybody pays for it at some level another, but if we don't get to have those kind of narrative translation in conversation, that things weren't ever changing, at least a transformative way that's necessary for our young people to thrive and really reach their their best.
27:38
Next slide, please.
27:41
As far as I've sort of, you know, really lay down for the, the, the few things I wanted to kind of share with you all is that, again, I'm probably speaking to the choir. So for all of the sort of, tertiary hundred plus people that signed up and probably listening right now, is that, you know, when I think about young children, ensures, development over the life course, is that we have to recognize, right?
27:59
That there are peaks and valleys, right, then nothing is fatal, we do know is that for fortune to be healthy, there are things that are going to be really promoted, right. So we know that sort of the home environments that's promotive, this affirming, sensitive, this responsive, but also the healthy in many ways, whether it's spiritually physically has the economic security that those are going to play, showed it at a stronger odds, especially in the first five years of life. When the brain is developing, when language development. That that places children at a higher odds of having a successful life, right. Now, compare that to children who may well experienced and housing insecurity. Economic hardships, a different levels of trauma and early childhood adversities rate that those children are sort of, you know, likely on a track or potentially not reaching their potential.
28:47
Again, I want to remind us that, especially for me as early child person, we know that the brain is plastic. We know that children are resilient, right. And so it's not fatalistic. When I say that, Yes, you may be living in poverty. As I was a kid, or, you know, doing a lot of different trauma, that doesn't mean that you're going to have a horrible life, but It does make it a little bit harder. And so, What did we do to make sure that, during those formative years, they were doing as much as we can, in terms of policy work into the programmatic? In terms of research that supports, What are we doing? To ensure that children are able to continue the life course, in a way that's positive and optimistic, but really, it's, surely, they go to Thrive and live into their sort of, older adult years.
29:25
Next slide, please.
29:27
But it for me, is really important.
29:29
And again, I'm not gonna do a history lesson here, but, but I wanted to make sure that we all understand the, in the previous speaker really spoke a little bit to the right that things are not felt similarly right? Whether it's gun violence, whether it's mental health, but it's Coburn and teen, right? They're not felt the same across various racial ethnic groups. But for me, is the point that we really call out. How does raise an impactful is healthy development. And so, what you see in front of you is, of course, the academic will always have something complicated. But don't worry I'm going to uncomplicated shortly. But basically that's the framework that we created in late last year to really communicate the different forms of racism, right? We have, when people talk about the water, right, the water that the worst women and is really be the white supremacy is really bad and cultural racism. That means that we're really that the things that are viewed as white or whiteness are viewed as more superior. Those who look white, or what I like to have, the best outcomes in terms of education, economic drivers, for the most part, health, and other social indicators. And that's because the water just continues to turn that out.
30:31
But that's because of the structural racism that we have pretty much debated into our education system into our house and into our labor markets, into our immigration policies.
30:42
And so, those structures really basically stratified people to have different kinds of opportunities over time. And, of course, other things like interpersonal racism, which we call bias discrimination, where it impacts how individual sort of interact with each other.
30:57
And so my whole point of really showing this digital artist to say that racism in many forms, a compound in different things, right, so for young children, right, they can be impacted by the kind of early care and education environment they're in.
31:10
They can be impacted by the adults and educators around them. They could be impacted by the neighborhoods that had been disinvestment under invested in or the ballots within those neighborhoods that could be impacted by the structural, sort of breaks them in terms of the kind of access to academic support, access to sort of educational opportunities that are high quality. Right? So, again, imagine that that's sort of the compound in nature, raised them. That impacts healthy development, again, whether we're talking about physical development, social emotional development, and mental health. But we have to begin to uncover all of these forms of racism that really impacts and healthy development. At the same time, we're thinking about inter generationally for young children to impacted by things before they're born.
31:52
And then, obviously, after the importance of what about issues of lead poisoning, issues of toxic and vicarious racism, those impact children's healthy development, either directly or indirectly, right? Whether you're the parent, the mother, or the birth in person, and just sense, wouldn't let it all sort of things. It impacts children's healthy development over time. But, I want to also make sure that I sort of also elevate the cultural assets that many families and communities had, right? Even if you're living in poverty, even if the Emitted DISA two spaces, we wanna make sure that we'll call attention to the kind of assets and many families and bring them. For example, the different kinds of language system that people bring when they're trying to communicate with those who are in their community, or those in their cultural groups, or the kind of aspiration that many people have. Right. The fact that you may be living in poverty, but you still aspire to greatness of education and many other things, even when it's probably, sort of a hard road to get there.
32:50
So, we have to begin to, sort of, elevate the kind of assets, communities, and children and families have, because we often look at them. But the logical lens, which is not helpful, We try to humanize people. So, this, what we call rise framework is really trying to make sure that we are able to articulate what is raised them in different forms. What does this impact on children's healthy development? But, what are the cultural assets that families bring in many ways? And, we shouldn't continue to ignore those level of assets, and we have measures of cultural assets and ... on, but these are just just to make sure that we're able to see the full humanity.
33:27
Next slide, please.
33:31
So just to sort of you know, I've done a lot of work and a lot of papers and particularly, you know we've done a whole series of on black babies, Every project funded by Pritzker. And you can see the QR, according to, when you would take your code, you'll get a copy. You can see this report. And what we've done over the past 2, 3 years is to really elevate how black parents and their babies are doing. During the global pandemic of both Coburn 19 and racism, what we call the dual pandemics race racism has always been here, black them is that we'll use belted babies. You have always felt that some way or another. And so we're trying to really elevate this idea of dual pandemic rate. And the report that you'll see, is that a demonstrated that even two years into the Kubernetes pandemic black them is in particular and their babies are surviving, right?
34:15
Although they continue to fill the full weight of racism and discrimination, they're still being economically challenged among other kinds of inequities. And it's, there'll be compounded by the ongoing global pandemic.
34:28
And we know their racism and discrimination, which is often not discussed enough, and, especially when it concerns young children, that we know, is still a major concern for black families and their babies along the economic instability.
34:42
So for example, I'll share with you what a couple of data slides Next, slide, please.
34:47
So in the report there's a series of data slides: They'll compare black families to other non black families, and we have data for pre pandemic, so in this slide that you're looking at here, the darker shade of red is pre pandemic, and then the lighter shade is really March 20 21 is a little bit darker, and the lighter cause more retreat to.
35:06
And I should point out, that this data is collected through a collaboration we have with Stanford, and the rapid ..., which stands for Rapid Assessments of Pandemic Impact on Development in Early Childhood.
35:18
And so, as a series of questions around health, around economics, obviously, around placement discrimination, the part that the media team added and what you basically see here is that really one of the three black parents report their use of slurry directed at them during the pandemic.
35:33
This rate actually decreased slightly between 2021 and 20 22 and what you'll see across the board is that before the pandemic right, there was a high level of parents reporting. Many variations of discrimination, whether police mistreatment not being higher being called the slurry, weaknesses that obviously during a pandemic when maybe we'll actually locked away in their home trying to save for the most part. Depends on the black parents of babies, Reported a lower frequency of that, right. So, but, but we know it's still happen, it's just that now your interactions with other people are not happen as frequently, but we also noted in our data, that black parents also reported cursor's about unfair treatment of their children, particularly before the pandemic.
36:14
So then, this means that for families, for families with young children were talking about children under the age of three, that even that early in their their life, parents are recursive about how the child wants to be treated based on opportunities being provided. Would they be unfairly punished? And so parents are really already acutely aware that the black child is likely to have these experiences.
36:37
We see a similar trend for our Latino and Asian families, not as high. But we see a similar trend with minority families are having this sense of concern about how their children as want to be experts in the world as they get older.
36:53
Next slide please.
36:57
And so what you see here is another part of the day that really begins to call out, that even as we went into the second year of the pandemic, that, even over quarter, black them at the poverty of 22.
37:07
Work students in Material hardships again, read them on material harsher. We're talking about things like pay for utilities, housing, food, education, like childcare health care, Right? There are many themes are not able to do that, and that also includes Black families and middle income families.
37:24
And so that's something that we have to continue to sort of, I think, push on, is that even we think that your middle income should be fine for black them as who live in sort of economically vulnerable sort of position, And, right? But as they say, when they raise for certain communities for black, that means a pores, right? Is that same idea that even if you're middle class or middle income for Black families, you are still economically vulnerable.
37:47
And, see, we can see in our data, that that over 10% of black families who are middle income will experience an almost three or more mature hardships, meaning they couldn't pay for housing, for food, for utilities. And, again, that has detrimental impact on the function and a psychological well-being of families, but also their children over time.
38:08
Next slide, please. So, I mean, so the reports show a whole lot in terms of economics in terms of health and stress, in terms of the sort of depressive symptom knowledge, the parents of reporting. And we know those have implications for children's healthy development. And so, I encourage you to look at the reporting and series of other reports that we have really about black families and their babies. And I will note that we, that we also have a report around in the child tax credit. And how those actually helping families reduce his stress for black families to have babies, as well as like being a family with babies, right? That the child tax credit, in particular was really powerful for black and Latino families in a reduced level of stress, the level of depression, and loneliness, right? And so we cannot sort of underscore how important some of our policies could be for many more generalized families.
38:59
So, as I sort of, you know, leave, extorted, what are some things that we can begin to do, right, I could have shared so many more data.
39:05
But I wanted to leave you with, like, what are some things that we're seeing that that's really important, and it could potentially, really be helpful is according to help you did on the children. And so I think about it from a three piece perspective, right, So, three piece of protection, promotion, and preservation.
39:19
So the first P is how we ensure that children families are free from harm, trauma and adversity, like, what do we do to do that basic protection?
39:27
The second is promotion rate.
39:28
Holly foster insurance health way, including a physical health, their mental health, their social emotional health, all of that how we fostering their health, would also their wealth, right? We talked a lot about how people we don't talk about, well, which is something that you are over generations, right? So how do we foster wealth? And it obviously access to educational excellence and it. Finally preservation, right? We know that for a lot of the mental health challenges overseas, we know that people who children and youth are not feeling connected and seen invisible, that's impacting their sense of self.
40:01
So how we preserve and their family, their culture, their land, right, their language, and their families, and identity in many Meaningful wage rates. So how would you what I call the three P's and so I'll just briefly next, next slide, please.
40:16
So in terms of using the three P's, along with the National Black Child, the Institute, the foremost Civil Rights Organization for Young Black Children, did, we create this What we call the Black Child National Agenda, that really talks about, what are the policies that we at least see working in many sectors, at least in many states across the country, that we think it's going to really improve the health, the wealth and well-being of black children. And really, we argue fusions for black children in black communities. This will actually benefit all children them as a community because of how much focused on really those safety nets and the things that really matter. Right. And so I'll talk about them within the three P So the black China has had policies that we no evidence has shown is really impactful for their health and their wealth and many other well-being outcomes. Next slide, please.
41:08
If we take a look into the blockchain agenda, crossword the three Ps. I want to just flag sort of like the sum of the how they connect, right. So, if we think about protection policies, we know that we have just showed that. Families are really free from racism and discrimination, but also, material hardships. That means things like maintain a child tax, credit, income, supports. We've seen that have been very beneficial for our children's healthy development. We also have to address harsh enough their discipline. We continue to see the black children, native children, and children with disabilities are likely to be harshly disciplined, and suspended expelled at a much higher rate than other children. So we have to figure out what policies to ensure that children are having the best expresses the early education. Access to early intervention, right? Especially education.
41:52
Many black and native children are like it's important to be born pre-term and low birth weight. And so how do we think about those issues?
41:59
And then, finally, promotion.
42:01
Our policies around racial wages, wage gap, Family Medical Leave Act, expanded health insurance, and extra care education, and family preservation, right? How are we? Making sure that we're investing in black, owned, and black led businesses. How do we show our culture responsive curriculum practices? And really, how do we pass reparations. Right because the end of it we have to continue to preserve communities to ensure that children are healthy and thriving.
42:27
And the last slide, please, next slide, please. And so really, as I started to take into account, how do we continue to do this? How do we make sure these policies not just localized? We're really statewide and national, right? I argue we have to continue to engage in community partner learning. We have to think about it. We do Black Babies Awareness Month and work with the black media. We have the Black Child Agenda. We have to look at, really on national studies. Do they address racism, sexism, classism, and all those kind of things. And we have to continue to mentor our younger people.
42:58
Next slide, please, And we have to think about how we change the water inactivated change. And this is an example of when we did our awareness month. This means that we have to connect with the communities where they are, right? Whether is local media, whether it's sort of social media feeds, how do we continue to push information that's really going to ensure healthy development of children and families? And so, just the last slide, the last couple of slides, I want to just flag, right? again, if you go to the website, you'll see a slew of resources, really. We take our, all of our peer reviewed articles, and we try to translate the policy and practice again. We can I make a change without actually making sure that gets translated to those who need that. And then finally, you can click to the next two slides me.
43:42
Please, again, look after the new book we have coming out. And then finally, I'll just say, obviously, when we get to that, feel free to follow me on LinkedIn and Twitter, And of course, we have the website as well. So with that, I'll pass the mic back. Thank you.
43:59
Thank you so much, doctor Rocha, for making clear the devastating impact of discrimination over the life course, on our children, and how important correct policies are in Community Action to make a difference. Hopefully, we can address that if we have a little time, more time for questions after this next presentation. Next, we will hear from doctor ... Patel, MD. Doctor Rob Patel is the AVP and Senior Medical Director at Blue Cross and Blue Shield of North Carolina. She is responsible for the evaluation of medical necessity, appropriateness, and efficiency of the use of health care services, procedures, and facilities under the provisions of the Health Plan. Before joining Blue Cross and see she worked in private practice doing acute care and chronic pain management, she is also an advocate for protecting the mental health and well-being of children. Doctor ...
44:55
Patel will discuss Blue, Cross blue shells innovative strategies for approaching mental health through the community. Doctor Ralph Battelle.
45:06
Thank you, thank you for the warm and kind introduction. I appreciate it, and hello, everyone. Thank you for taking the time today to join this important webinar and thank you for and thank you to the NIH CM for having me today. And anecdotally, I was recently, if you go to the first slide, that would be great.
45:21
I was recently talking to my child's principal, who recently retired from, from her role, and we were talking about just some of these poignant issues that our two speakers were talking about, the struggles of children and youth today related to food insecurity lost mental health struggles. And I know, personally, as a physician, you can't just look at somebody or really even understand, just by looking at them entirely what's going on in that person's life. Especially when we think about children. Oftentimes they don't come out and say, You know, My dad drinks a lot, or I don't have enough to eat, or, I feel less adequate. And so it's important that we continue to have these conversations and talk about this and continue to de stigmatize mental health and that's how we do it is by talking about it and by bringing education and awareness to it. So can go to the next slide.
46:13
So as I mentioned, this topic is so timely, not because the well-being of our children's mental and physical health is a new one. It's because there's such an urgency about it right now. one news story after another has made it clear that our children are facing a monumental crisis when it comes to their mental health.
46:32
Earlier this year, the CDC released a heartbreaking report which showed that feelings of hopelessness and despair were increasing among all of our adolescence.
46:43
And really more than half, nearly three in five adolescent girls felt persistently hopeless or sad.
46:50
And while all teen's reported, increasing, mental health, challenges, experiences of violence, and suicidal thoughts, and behaviors, we heard a lot about this as well. That girls actually fared worse than boys on all measures.
47:04
Next slide, please.
47:07
So in my state of North Carolina bays, a North Carolina Child Health Report card and it tracks key indicators of children's health and well-being in four areas. It's Healthy births: Access to Care, Secure Homes, and Neighborhoods and Health Risk Factors. And this report provides data on drivers of health, such as access to health care, graduation, date, great rates from school, risk factors such as asthma, teen births, infant mortality, poverty, child deaths.
47:37
And more than one in five high school students have seriously considered suicide. We heard about suicide rates going up from my, from my colleagues, who spoke before me in 20 21, up 16% from 20 17.
47:51
And the diagnosis of mental health concerns are also on the rise more than, one in ten children. Ages 3 to 17 in North Carolina had a diagnosis of depression or anxiety in 20 20, which was almost a 50% increase from 2016.
48:06
But the good news, if there is any good news about those stats, is that we are talking about this more openly as a nation. We're talking about youth mental health and as I mentioned earlier, we need to continue to keep open dialog. one of the challenges I would say is that there's no one size fits all approach to addressing these needs.
48:24
And in fact, we can't talk about a child's mental health and well-being without talking about the child's caregiver's well-being and mental health.
48:35
Young people don't just face individual, social, and economic and academic challenges that we've all dealt with right when we were young, but they also take on the traumas of their parents and caregivers. And for the past three years, as we've gone through cover, those traumas have been especially significant.
48:53
So really, addressing mental health challenges in children requires a whole person, whole family, whole community approach. And I'll talk about that shortly.
49:04
If we can move on to the next slide, if we could just hang onto this slide for just a bit, when we talk about stressors, and we've heard stressors mentioned several times, young people were already experiencing significant behavioral health challenges before the pandemic disrupt disrupted our lives on so many levels. And you take social pressures, the usual social pressures that we've all dealt with, and you disrupt social networks.
49:29
And then you completely twist the system and make it even worse. So children have also been dealing with profound levels of grief and loss. In fact, more than 250 children in the United States have lost their primary caregiver as a disruptive, direct result of covert.
49:45
They've also lost peers, their teachers, faith leaders, neighbors, other loved ones.
49:51
And that's nothing to see, to say of the children who have had their family torn apart Because the factors indirectly related to the pandemic we talked about, and we heard about the rise of substance use disorders, 40% of the children in foster care system are there because the parents misuse of drugs or alcohol, and the pandemic also introduce things like unemployment, financial insecurity in households, which also increases the risk that the child will face, abuse, neglect, or absorb the parental stress in other ways.
50:20
And when we talk about health impacts and the long term impacts of this, things, grief, parental separation, substance use, that I talked about, physical abuse, neglect, those are just a few examples of what's listed here with adverse childhood experiences. And those effects we know can last a lifetime.
50:38
According to the CDC, in fact, nearly 3 of 4 high school students reported one ace or adverse childhood experience, and one in thirteen experience experienced four or more aces during the curb and 19 pandemic.
50:52
Students who face trauma often find it more difficult to engage with their schoolwork.
50:58
Aces are linked with anxiety, depression, disruptive behavior. These challenges with cognitive impairment and self-esteem can continue on into adulthood, and that undermines family structures, employment, health, and well-being, and once a child has accumulated six of these aces, they stand to lose 20 years of their life expectancy on average. And on top of these universal challenges, some communities take any pressures, we just heard about that, young People of color, LGBTQ, plus teens, rural communities.
51:30
Next slide, please.
51:34
one of the significant challenges, we feel her feel here in North Carolina, and, again, it's not unique to our state. We heard this with our first speaker is the lack of Qualified Health professionals. This is the map of the Health Professional Shortage. Areas. Are the HPSA, which is put together yearly and refresh by North Carolina, DHHS.
51:53
North Carolina has 100 counties, 78 of them are designated rural counties, 91 of them are designated Rural Health Professional Shortage Areas across three major areas of health care, primary care, dental, and medical, and mental health.
52:09
So we have to keep sight of the fact that this isn't just an issue that affects physical health. A few, few realize and recognize the severity of our access to mental health here in North Carolina. That pandemic has driven greater demand for mental health care but many North Carolinians didn't know where to turn for help.
52:26
But it's important to understand that building a more robust workforce to handle our state's growing need for health and clinical care is only part of the problem. People face barriers long before they try to book an appointment or even walk through the door of a provider's office.
52:41
Next slide, please.
52:46
And really, to summarize what I was just talking about, mental health problems are not adult problems. Depression, anxiety, and other mental health challenges can show themselves as early as age three.
52:58
Unfortunately, treatment for most of these doesn't begin. Well into adulthood, usually 6 to 23 years after symptoms first appear.
53:07
Unmet met mental needs will impact a lifetime. Putting children at greater risk of academic and social challenges likely escalating into more serious mental illnesses. In fact, roughly half of all adult, serious psychiatric disorders first appeared during childhood or adolescence.
53:25
And so, really, when we think about this, no child's future should be written in stone or is written in stone. But Strategic direction now will help ensure that more children's needs are addressed, and that they stay, on course, for a healthy and rewarding life ahead.
53:41
And as I, as she, as a speaker, mentioned, I work at Blue Cross, and we have a specific way that we're trying to address this. And understanding that action must unfold on multiple fronts, So finger to the next slide on the whole person approach.
53:56
We really need to understand and start thinking in terms of mental health versus physical health, or just health.
54:02
So, both of them are intertwined and unsufferable, some of the things that we've done we have prior towards access to primary care and mental health care providers through Telehealth. We've collaborated with a company called Headway, which is to expand our network of behavioral health providers with a specific focus on improving access to care for children and adolescents, especially in these rural and social revolt, socially vulnerable counties.
54:28
one of the more critical components of this effort is how we're integrating mental health and substance use treatment into primary care, because we know there are not enough mental health and substance abuse providers to meet the demand. So, we've made it a priority to invest in ways to reward primary care providers who are attuned and ready to respond to their patients, mental health needs. And this can really, as I mentioned, identify potential risks before they escalate into crisis. We also have internally a dedicated team of care navigators, and they match members experiencing mental health needs with providers who can provide that ongoing support.
55:05
On our next slide, when we talk about the whole family approach, as I mentioned, supporting a child's mental health needs means supporting the caregiver and the family more broadly. And we try to meet members where they are on that continuum health of health care needs. So we've done a lot to address and fight the nation's opioid epidemic. We heard some of the stats around that. By participating on the President's Commission testimony to the Senate, we've invested in prevention and treatment that benefits everyone, not just families who are involved directly with substance use disorders.
55:36
And we really need to look at a holistic approach and system of care that emphasize as positive outcome comes in the form of family continuity and security, because that's what brings and builds the stronger communities.
55:49
So, Healthy Blue is Blue Cross as Medicaid program. We've done such a thing to launch an evidenced based model, family centered treatment, and that will provide long term stabilization with families, with youth who moved, who moved the between child welfare and juvenile justice systems. And they could be at risk obviously of unfavorable and traumatic situations such as being removed from the home.
56:11
An example of some exciting work at a national level that's being done to promote healthy childhood development by integrating family well-being into the pediatric centered care setting is Reach Out and read.
56:23
And that's a national program, and that provides, it gives providers books. They're called Prescribed books to help caregivers who have limited resources and access to reading materials to share with their children.
56:37
Next slide.
56:40
When we think about a whole community approach, it's important to think on two levels, so we have to think, what can be done to support the community's capacity to respond to this mental health crisis and to how do we leverage local opportunities? And the boots on the ground expertise to have a broader impact. So, for example, at my company, we committed $2 million to support 11 community based organizations to expand pathways to mental health and rural and underserved areas. There's also a better need and a stronger need to equip health care professionals, social service providers, educators, and community based organizations to develop and deliver trauma informed care. We need to support children in foster care and their families. We want to support children, they are very high risk of entering the foster care system, are going into a group home. And the goal is to really change that families trajectory with intensive support, new parenting and communication skills, and evidence, and strengths based mental health intervention services.
57:38
And finally, outdoor exercise, it's it's definitely worth emphasizing the importance of investing safe spaces for children to play outdoors. Green spaces and play spaces are not equally distributed. In many cities and towns, families living in affluent areas have greater access to parks and green ways and community gardens. These areas are scarce in many rural areas and historically underserved communities, sidewalks, parking, parking lots do not offer the same opportunities for safe and imaginative play. So when we think about the health benefits of outdoor activities, physical fitness probably comes first in line, but data clearly shows that it also yields psychological benefits, and things that we don't just get from going to a gym.
58:21
Last slide, please.
58:24
So, finally, I'll just add that working in silos will not solve the challenges that our children face. It will not harness local resources that each community can bring to the table as a local company, Blue Cross actually has roots in the states that we serve. We are based in North Carolina. We have service and all 100 counties and our presence is essentially remain steadfast since 19 33, but we still, we learned that there's a lot more to learn and to explore. and every day we solidify our connection to the state. By, by listening and acting on what we hear.
58:56
And this is what is displayed here, is this extra miles tour, where our leaders have gone and are going to all 100 counties across the state to understand what are, what are the struggles of the counties? Are the boots on ground people doing the work? How can we leverage what we learned in one part of the state, and utilize that in another part of the state? So we're discovering the possibilities and brainstorming new strategies to really improve the health of rural, underserved communities. And that's really the essence of the work that's ahead, right? It's Turning the tide on Youth Mental Health. And that demands listening, and sharing, and collaborating and with our children, our families, across our communities.
59:34
So, I appreciate your time today, and thank you very much.
59:41
Thank you so much doctor Route Battelle for sharing Blue Cross's strategy and for that holistic and compassionate approach to child mental health. We are going to try to stay on just a few minutes to take just a couple of questions are, many questions that have come in today have been about how do we influence policy and how can we influence policies that might change some of the many circumstances that we discussed today. Doctor Wolf, I would, I would ask you to start and there are many questions about how do we influence firearm related policy extent that hold on to the extension of Medicaid that occurred during the pandemic get people to use evidence? Instead of opinions, doctor Wolf, would you want to begin.
1:00:35
Oh, that sounds like good ideas to me.
1:00:37
I'll just single out firearms for the moment, it it's a very difficult time with us, you know, very potent ideological divide in our country, on, on an issue that's very volatile.
1:00:55
It's frustrating, though, that even the simplest laws to limit children's access to firearms Go down and defeat in many state legislatures, simple things like having locks on guns or, or safe storage of ammunition is, is, is defeated.
1:01:16
So we can have our debates about whether adults should have access to guns, but, if even simple measures like that are defeated.
1:01:23
We, it's getting it to be a bit unacceptable at a time when all cause mortality rates are now increasing.
1:01:32
When I say all cause mortality rates are increasing at ages 1 to 19, it means that the chances of our children surviving to age 20 are now decreasing.
1:01:40
So at a time, when our children are less likely to ever become adults, I think it's it's time to do something sensible about policy.
1:01:47
That said, I've been criticized for talking about simple measures like that because most children who are killed by guns, the shooter is an adult.
1:01:57
And so we do have to confront the issue of the widespread access to guns and increasingly lethal guns among adult owners as well.
1:02:09
There's much more to be said about dealing with mental health issues and dealing with structural racism, but time is short, so I'll leave it with that.
1:02:18
..., again, in your work, critical policies, maybe expansion of child tax credit, Medicaid, other things that you think might make a difference?
1:02:29
I mean, I mean, I think, Absolutely. I think at the end of it, right, cheated policies requires a whole lot of shift, right. And that's why I think I talked earlier about the importance of sort of kind of narratives. And really being able to translate our research and evidence based findings in ways that are accessible, right? Again, not just through our articles, but due to weather reports, whether it's hosted webinars like this, talking to our neighbors, and, of course, voting. I think we can't ignore the power of being able to vote and how that's actually be limited across many communities, particularly black and brown communities. And so, I think, I think, for me, it's just how do we make sure that we begin to identify where our policies, child tax credit, actually happens in red and blue states, right? So, there's certain policies that we're seeing across the board, regardless of ideology, that we know benefits families, like, you know, healthcare expansion, finally explained here in North Carolina, right?
1:03:21
So, there are things that we know that are happening that doesn't have to have this ideology states, but we know it happens over time. It requires a lot of advocates, but also voting in a smart way.
1:03:36
That's your ram Patel. Did you want to add something?
1:03:40
Know, I was gonna mention exactly what doctor Rick was making.
1:03:44
Reference to is the fact that it's, it's important that we all work on this together. And the fact that Medicaid expansion has finally happened in North Carolina. I think it's important that we continue to evaluate and look at our policies.
1:03:56
We also have several questions that have come in about the role of social media. I am not sure that that's within your expertise. And I will feel that to all three speakers, there is concern that social media is contributing to many of the issues we're talking about here today, including Child mental Health. Perhaps, doctor Ravitch, how you're nodding, so perhaps you might take that one.
1:04:18
Now, I just, I smile and laugh because that struggle is real in my own home. To get my children, to get off devices and get off the shelf, So, Yeah.
1:04:27
I mean, you know, covered years definitely, we saw an increased reliance on social media, I think, the last statistic I read among adolescents and young adults, about 90% of them use one or more actual social media platforms, and And you're right. There's data that suggests a correlation.
1:04:46
Between said, it's social media use and a wide range of mental health and physical problems, including depression, obesity, unhealthy eating sleep disorders, substance use disorders, body image issues, physical inactivity, and then FOMO, which is, you know, having unrealistic expectations about life and what people post often being taken as truth.
1:05:09
Because, of course, if it's if it's posted online it must be true, right?
1:05:15
And so, I think one of the things I read about the most was there's now a big trend of people using these social media platforms. I think, especially maybe tiktok, where people are self diagnosing, which is also a concerning thing, and of course, there's nothing wrong. I don't want to, you know, completely say that everything is either good or bad. There's nothing wrong with, I think, gathering information about issues with, you know, things that people may be struggling with online.
1:05:43
But I think it's, and I think it's also, I think it's also great that people are sharing their own challenges, because I talked early in my talk about de stigmatizing and how it's important to speak openly about mental health. And, and that makes people feel less alone within their own struggles and their diagnoses. And so these kinds of posts, and certainly rare, raise awareness.
1:06:04
But everything, you know, again, symptoms and disorders and everything else looks different in every body.
1:06:10
And so it's important to not sort of label yourself or diagnose yourself based on somebody else's experiences or symptoms. And so sometimes, you know, social media posts can certainly lack credibility, so it's important to recognize, you know, kind of fact from fiction.
1:06:30
Did anyone else want to address that?
1:06:32
Conundrum? I'll just, I'll just add, from a slightly different perspective, because I agree with everything that's been said about the harmful effects of social media on children.
1:06:41
But also to say that social media is becoming toxic for rational policymaking, and I say that simply because we're awash in a sea of misinformation.
1:06:54
Currently, my gray hair indicates that I come from a time when we relied on peer reviewed research for scientific evidence and publishers and so forth, to that information that we we used for references.
1:07:10
Now, amid conspiracy theories and all kinds of other content on social media, it's very hard to have a rational conversation about what the facts are and to have, you know, data informed decision making, it ever, national, state, or local level.
1:07:27
So I think an immediate challenge is Tucker.
1:07:29
Doctor Rocha said is translating the evidence in ways that speak to people and meet them where they are and communicating the facts of the situation in a more effective way.
1:07:41
That's Erica, Did you want to add anything?
1:07:44
Not that I need to add as having two young kids, like that the rap about? I mean, I'm fighting social media. I will say, obviously, it's not binary. Like, we know that social media has had some positive bring community together. So, but, again, it is really how do we use it? And how do we make sure that we're addressing the misinformation and disinformation that actually is targeted Particularly black communities and Latino communities, Especially on a deep level. So, I think we just have work to do, and how do we use some of these tools at our fingertips in ways that's really promotive of our health in many ways. And we just haven't figured that out yet.
1:08:22
Unfortunately, that is all the time we have today. I want to thank our panel. You're all extraordinary speakers and covering such a broad and challenging issue. We really appreciate you sharing your valuable work. Thank you to our audience for joining us today. Your feedback is very important to us. So there'll be a survey popping up after the event. Please let us know how you feel about the event. And check out some of our other resources on our website. Again, my thanks to all.
Presenters

Steven H. Woolf, MD, MPH
Director Emeritus and Senior Advisor at Center on Society and Health, Professor in the Department of Family Medicine and Population Health, & C. Kenneth and Dianne Wright Distinguished Chair in Population Health and Health Equity at Virginia Commonwealth University

Iheoma U. Iruka, PhD
Founding Director of Equity Research Action Coalition & Faculty Fellow at University of North Carolina at Chapel Hill

Anuradha Rao-Patel, MD
AVP, Senior Medical Director, Blue Cross and Blue Shield of North Carolina
More Related Content
See More on: Health Equity | Behavioral Health